Introduction
The Bonebridge hearing implant is a novel active bone conduction technology designed to treat conductive, mixed, and specific forms of single-sided deafness (SSD). In contrast to percutaneous bone-anchored hearing aids (BAHAs), the Bonebridge is entirely implanted subcutaneously, delivering vibrations directly to the inner ear by bone conduction. This method reduces skin problems and improves aesthetic results while delivering efficient auditory rehabilitation.
For audiologists, ENT surgeons, and rehabilitation experts, comprehending the mechanics, indications, surgical techniques, and clinical outcomes of the Bonebridge is crucial for patient selection, counseling, and long-term management. This page provides a thorough overview for specialists in the domain.
Mechanism of Action
Principles of Bone Conduction
In typical hearing, sound waves access the cochlea through the air conduction route via the outer and middle ear. In instances of conductive or mixed hearing loss, this route is impaired. Bone conduction circumvents the external and middle ear, transferring vibrations straight through the cranial bones to the cochlea, and triggering the auditory nerve.
Active Bone Conduction with Bonebridge
The Bonebridge technology distinguishes itself from passive devices, such percutaneous BAHA, by actively transmitting vibrations:
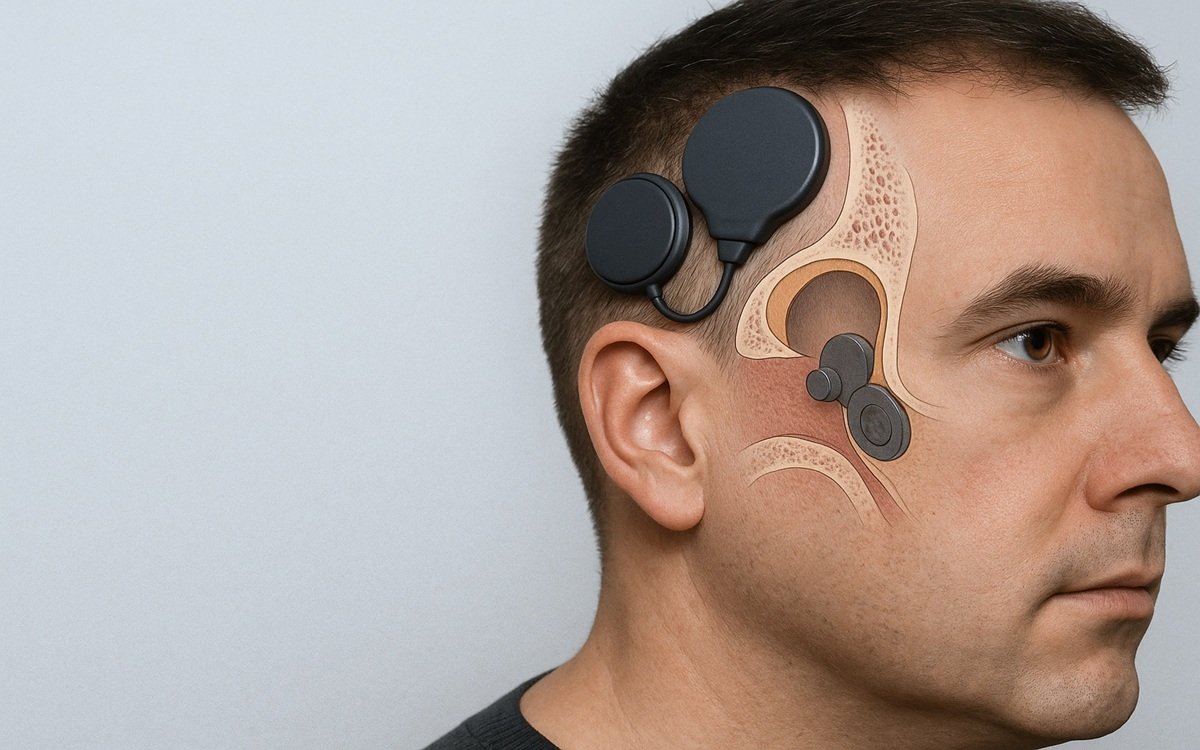
- External audio processor: Captures sound, processes it, and transmits signals transcutaneously through an inductive link.
- Implanted part (BCI – Bone Conduction Implant): Receives the signal and contains an internal actuator (floating mass transducer, FMT) that generates mechanical vibrations.
- Bone vibration: The FMT transmits vibrations through the skull bone to the cochlea of the implanted side (or contralateral side in SSD cases).
The system’s complete implantation beneath intact skin mitigates skin-related issues and facilitates more inconspicuous usage in comparison to abutment-based systems.
Indications for Bonebridge Implantation
Bonebridge implantation is appropriate for individuals with conductive or mixed hearing loss, as well as for specific instances of unilateral deafness.
Conductive and Mixed Hearing Loss
- Patients with chronic otitis media, canal atresia, or ossicular malformations that preclude or limit the use of conventional air-conduction hearing aids.
- Bone conduction thresholds typically should not exceed ~45 dB HL (depending on implant generation and manufacturer specifications).
- Provides improved speech understanding in quiet and noise, compared with unaided or conventional solutions.
Single-Sided Deafness (SSD)
- Bonebridge can reroute sound from the deaf ear to the contralateral functioning cochlea.
- Improves speech understanding in noise and spatial awareness, though binaural hearing restoration is not possible.
- Beneficial in patients who cannot adapt to or prefer alternatives to contralateral routing of signal (CROS) hearing aids.
Pediatric Considerations
- Approved for use in children depending on skull bone thickness requirements (generally >5 mm for implantation).
- Alternative solutions such as softband devices may be used in younger children until bone maturity is reached.
Candidacy Evaluation
The selection of patients for Bonebridge implantation necessitates a multidisciplinary evaluation:
- Audiological testing: Pure-tone audiometry, bone conduction thresholds, aided and unaided speech perception tests.
- Medical evaluation: Assessment of middle ear status, chronic infections, and anatomical considerations.
- Radiological imaging (CT/MRI): Used to confirm sufficient bone thickness and evaluate mastoid and temporal bone anatomy.
- Counseling: Ensuring patients and families understand benefits, limitations, and rehabilitation needs.
Surgical Techniques
Bonebridge implantation necessitates meticulous surgical planning, usually conducted under general anesthesia. The predominant methodologies encompass:
Site Selection
- Mastoid placement: Common approach when bone thickness is adequate.
- Retrosigmoid or middle fossa placement: Used when mastoid bone is insufficient, especially in children or patients with altered anatomy.
Surgical Steps
- Creation of a bony recess for the implant housing and actuator.
- Fixation of the device to ensure stability.
- Preservation of surrounding structures, especially dura and sigmoid sinus.
- Closure of the skin with the implant fully covered.
Surgical Challenges
- Adequate bone thickness is essential to house the FMT.
- Risk of injury to adjacent neurovascular structures (dura, sigmoid sinus).
- Requires preoperative imaging and careful planning.
Clinical Outcomes
Audiological Outcomes
- Speech recognition: Significant improvement in speech understanding in both quiet and noisy environments has been documented in adults and children.
- Functional gain: Studies report average functional gains of 25–35 dB HL, depending on configuration and patient-specific factors.
- SSD outcomes: Improved speech in noise and subjective benefit, though localization remains limited.
Quality of Life Outcomes
- High levels of patient satisfaction have been reported, particularly due to improved cosmetic outcomes and absence of skin complications compared with percutaneous systems.
- Improvements in social interaction, workplace communication, and overall hearing-related quality of life.
Pediatric Outcomes
- Children demonstrate significant improvements in speech perception and communication skills, particularly in educational settings.
- Early implantation provides advantages in language development and social integration.
Complications and Considerations
Bonebridge implantation is typically safe, exhibiting comparatively low complication rates. Possible concerns encompass:
- Surgical complications: Injury to dura or sigmoid sinus, though rare with careful planning.
- Device failure: Occasional reports of hardware malfunction, requiring revision surgery.
- MRI compatibility: Modern devices allow MRI at 1.5T or higher with specific precautions, but imaging considerations should be discussed preoperatively.
In comparison to BAHA, the Bonebridge presents reduced incidences of skin infection and revision surgery, hence enhancing long-term tolerance.
Role of Audiologists and Rehabilitation Professionals
Audiologists are central to Bonebridge management:
- Preoperative evaluation: Conducting audiological tests and counseling patients.
- Postoperative activation: Programming and adjusting the external processor for optimal outcomes.
- Rehabilitation support: Guiding patients through adaptation, providing communication strategies, and monitoring progress.
- Long-term care: Regular follow-up for device adjustments, troubleshooting, and counseling on realistic expectations.
Future Directions
Ongoing developments in Bonebridge technology aim to:
- Reduce device size for easier implantation in children and complex anatomies.
- Improve actuator performance for higher output and broader fitting ranges.
- Enhance MRI safety and compatibility.
- Integrate advanced connectivity features for wireless streaming and bimodal solutions.
Conclusion
The Bonebridge implant signifies a notable advancement in bone conduction hearing solutions, offering efficient auditory rehabilitation for those with conductive and mixed hearing loss and unilateral deafness. The active, transcutaneous architecture provides notable benefits compared to percutaneous systems, such as fewer skin problems and enhanced aesthetic results. Successful outcomes necessitate comprehensive candidate assessment, meticulous surgical planning, and sustained rehabilitative assistance from audiologists and interdisciplinary teams. Through ongoing innovation, Bonebridge technology is set to broaden indications and enhance outcomes for various patient demographics.
Leave a reply
Lets Talk.
Related Articles
Sound Therapy in Tinnitus
Introduction Tinnitus is among the most formidable conditions faced by audiologists. For certain patients, it constitutes a negligible background noise that may be disregarded. For some...
Know More >Introduction Tinnitus is not solely an auditory occurrence. Contemporary research increasingly characterizes it as a multisystem disorder encompassing cognitive, emotional, and physiological networks. Among the several...
Know More >Hearing Aids and Tinnitus
Introduction Tinnitus is a multifaceted auditory and neurological disorder defined by the perception of sound without an external source. Despite manifesting as ringing, buzzing, hissing, or...
Know More >
0 Comments
Leave a comment